Lung Cancer
Cancer is a disease that occurs when cells in the body begin to grow out of control. Canada has the 11th highest global rate of cancer. When cancerous cells are located in the lungs, it is called lung cancer. Lung cancer is the leading cause of cancer-related deaths in the world.
In Canada, it is the most commonly diagnosed type of cancer, representing around 25% of all cancers. Here, more than 21,000 people die each year due to lung cancer. In the United States, more than 131,000 people die each year. Lung cancer causes more deaths in the U.S. than breast, prostate and colon cancers combined.
Normal Lung Function
In order to really understand how lung cancer impacts the lungs, we must first understand normal lung function. The human lungs are sponge-like organs located in the chest. The left lung has two lobes and the right lung has three lobes. When you breathe in, air travels through your windpipe to the lungs. The air is divided into tubes (bronchi), and then into smaller tubes called bronchioles. At the end of the bronchioles are small air sacs (alveoli).
The alveoli are what absorb oxygen into your blood. They are also what removes carbon dioxide from the blood when you exhale. This is the primary function of the lungs – to oxygenate the blood and remove carbon dioxide from the body.
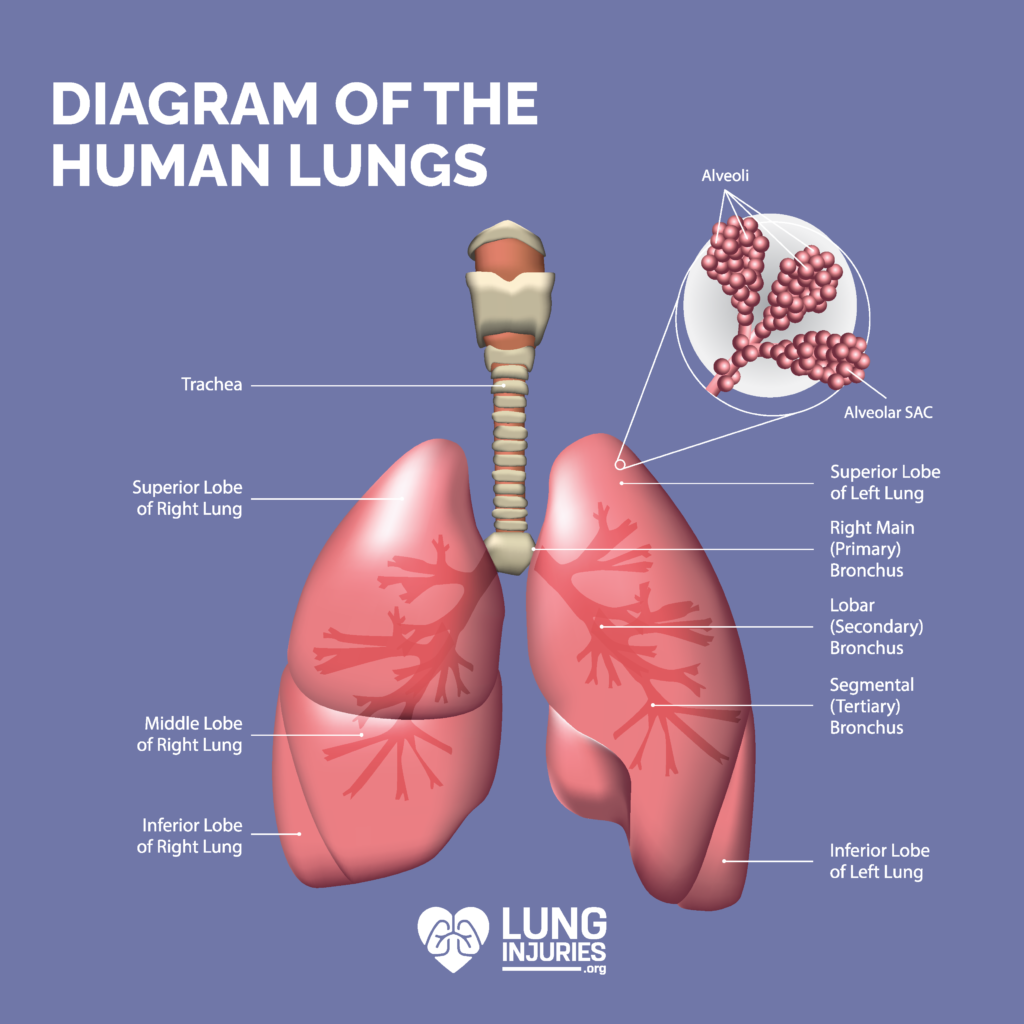
There is also a thin lining to your lungs called the pleura. This lining protects your lungs and helps them move against the chest wall during inhaling and exhaling. Below your lungs is your diaphragm, a muscle that forces air in and out of the lungs.
Lung function is tested by spirometry which assesses the mechanical function of the lungs, chest wall, respiratory muscles and airways. Spirometry is how your doctor determines your baseline lung function, evaluates how you are breathing and helps determine if therapies are working.
What is Lung Cancer?
Cancer causes cells in the body to change – even cells that are otherwise healthy. Normally, cells have a life cycle, and at the end of it, they die off. With cancer, however, cells continue to grow and multiply, which causes a buildup of cells. Then, those cells can cluster together and develop into tumors.
Lung cancer develops when cells in the lungs begin to divide uncontrollably. As a result, tumors grow and can impact lung function. For example, a tumor may be so large that it blocks a major airway. Tumors can also cause infections in surrounding tissues and organs.
Lung cancer begins in the lungs, but can spread to other parts of the body. It is categorized as either non-small cell lung cancer (NSCLC) or small cell lung carcinoma (SCLC). Unfortunately, most patients with lung cancer do not have symptoms until the cancer is advanced and treatment options are limited.
Non-Small Cell Lung Cancer
NSCLC is the more common type of lung cancer, with these variations occurring in around 80-85% of cases. Subtypes of NSCLC include:
- Adenocarcinoma: Most commonly develops in people who smoke cigarettes, or have previously smoked on a regular basis. It begins in the parts of the lungs that secrete mucus. Adenocarcinoma is the most common type of lung cancer among smokers and non-smokers. It is more common in younger people, and occurs more often among women than men.
- Squamous Cell Carcinoma: This type of cancer develops in the squamous cells, which are the flat cells lining the airways. This cancer develops mostly in the central part of the lungs near an airway. It is often linked to a history of smoking cigarettes.
- Large Cell Carcinoma: This type of cancer can develop in any part of the lungs. It grows and spreads quickly, and is more difficult to treat.
There are other subtypes that are incredibly uncommon, such as sarcomatoid carcinoma and adenosquamous carcinoma.
Small Cell Lung Carcinoma
SCLC is the more aggressive type of lung cancer, and occurs in only 10-15% of cases. There are two types of SCLC – small cell carcinoma and mixed small cell/large cell cancer. The name given to SCLC depends on the kinds of cells and how they look under a microscope.
Symptoms of Lung Cancer
Not everyone who develops lung cancer will have symptoms. Symptoms are either from the tumor within the lungs or from the spread of the tumor to either adjacent or distant parts of the body. Many patients can have seemingly unrelated symptoms such as headaches, seizures, and weight loss.
Sometimes, a tumor is found during an X-ray for something completely unrelated. Other times, symptoms develop, but only once the cancer has spread. The earlier you talk to your doctor about your symptoms, the better your chances are for successful treatment.
When symptoms do appear, they may include a variety of things that can be difficult to link to something as serious as cancer. Many of the following symptoms can also be linked to other medical conditions or diseases. Talk to your doctor if you smoke or have been exposed to carcinogens or radiation and develop the following symptoms that don’t go away:

How is Lung Cancer Diagnosed?
Lung cancer is most often diagnosed after the patient reports certain symptoms. If there is a possibility of lung cancer, a variety of tests may follow.
Imaging Tests
Next, screening tests are often done to see if there are visible tumors or other problems. These tests may include X-rays, magnetic resonance imaging (MRI) or computed tomography (CT) scans with contrast.
Imaging tests look for several things, including:
- Suspicious areas that could be cancerous
- If cancer is present and has spread
- If treatment is working
- To look for signs that cancer may be returning
Biopsy
Once imaging is done, your doctor may want to collect a sample of lung or tumor tissue through a biopsy. Often, a needle biopsy is performed during a CT scan. During this procedure, a long needle is guided to the area and a tissue sample is extracted. This sample will then be examined under a microscope in a lab.
Biopsies can also be collected by penetrating the wall of the bronchi or trachea to collect tissue. This is done during an ultrasound. Depending on the symptoms and other tests, doctors may perform a biopsy collecting only a small sample, or may attempt to collect a more aggressive sample.
There is also a procedure called a bronchoscopy, which involves inserting a small tube down into the lungs through the mouth or nose. A small camera with a light looks into the trachea and airways for signs of obstruction or abnormalities. Bronchoscopy is the best study for central tumors. It allows for direct visualization of the tumor and the airways. Biopsy samples can be taken directly from the tumor or from bronchial washings.
Lung Secretions
Doctors can examine lung secretions in a lab to see how the cells look. There are a few options for secretion tests, including:
- Sputum Cytology: Mucus coughed up from the lungs is collected and looked at in the lab. This test will often detect cancers in the major airways, such as squamous cell cancers. While it is quick and less expensive than other tests, sputum cytology is not as reliable as bronchoscopy or biopsy.
- Thoracentesis: Fluid that has collected around the lungs is collected for examination. A hollow needle is inserted between the ribs to drain fluid. The collected fluid is then examined in the lab. This test is helpful in determining fluid buildup that is malignant (cancerous) and fluid that is not. This test can also be used to drain the fluid, which takes pressure off the lungs and improves breathing.
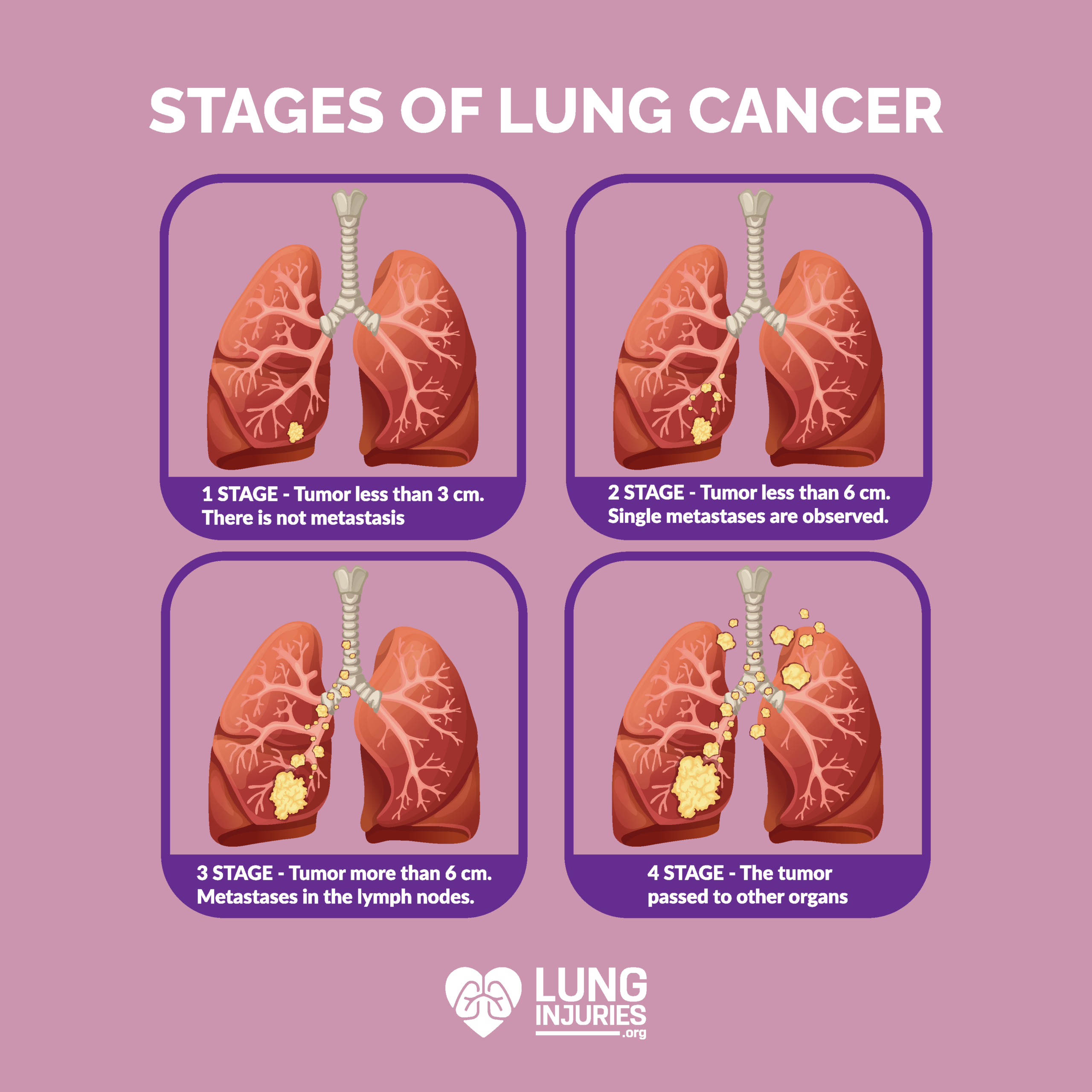
What are the Stages of Lung Cancer?
If you are diagnosed with lung cancer, your pathology report may include a “stage”. A cancer’s stage helps classify how serious the cancer is, and if it has spread to other parts of the body. Staging is the most important factor in determining a patient’s prognosis.
The World Health Organization (WHO) has a classification system for lung carcinomas. This classification system uses a histopathologic subtyping system that can better guide treatment. It also provides standardized terminology and criteria for diagnosis, which is important given that most people receive a high-stage diagnosis.
Staging Non-Small Cell
To stage NSCLC, doctors look at the following:
- The size of the tumor: How large it is and whether it is affecting nearby organs or tissue. The primary tumor is referred to as T. Tumors are then staged as T1-T4.
- Whether the tumor spread to nearby lymph nodes. Lymph nodes are referred to as N. NX means it cannot be assessed. N1-N3 denotes staging.
- Has the cancer metastasized? Has it moved to distant organs or tissue in the body, such as the brain, bones, livers or the other lung. Metastasis can be designated as MX, meaning it cannot be assessed; M0, meaning there is no metastasis; or M1, meaning there is distant metastasis.
Staging Small Cell
Staging SCLC is similar to NSCLC in that the goal is to determine how much cancer the patient has, and if it has spread. Doctors use a 2-stage system when staging SCLC – limited stage and extensive stage.
- Limited Stage: This stage means the cancer is only on one side of the chest. It is most often treatable with a single radiation field. Limited stage includes cancers that have multiple tumors in the same lung, or that have spread to the lymph nodes on the same side. Around one in three people with SCLC are in the limited stage when it is diagnosed.
- Extensive Stage: Extensive stage means that the cancer has spread widely in the lung, to the lymph nodes on either side of the chest, or to other parts of the body. Extensive stage cancer may also have spread to the fluid around the lungs. Around two out of three people who have SCLC are in the extensive stage when diagnosed. Sadly, extensive stage is largely incurable.
The type of lung cancer and stage will largely direct your treatment plan.
What are the Treatments for Lung Cancer?
There are several ways that lung cancer can be treated. Your lung injury treatment options will depend on the type of cancer you have, as well as other factors like metastasis. The possible treatment options include:
- Chemotherapy: Special medications shrink or kill cancer cells. Chemotherapy can be administered intravenously or can be taken orally. Some patients require both.
- Radiation: Radiation treatment consists of using high-energy rays to kill cancer cells.
- Surgery: Sometimes surgery is necessary to remove cancerous tissues from the body.
- Targeted Therapy: Drugs can be used to block the growth or spread of cancerous cells. These drugs may also be administered intravenously or may be taken orally.
In addition to these traditional treatment methods, there are also complementary and alternative treatment options, such as acupuncture, dietary changes, herbal preparations, etc. Some patients are also able to participate in clinical trials for cancer treatments.
In all cases, prompt initiation of treatment is important. Treatment decisions are often guided by the overall health of the patient and what is known as performance status which is also a gauge of activity level.
What is the Prognosis for Lung Cancer?
The American Cancer Society (ACS) uses a relative survival rate to help lung cancer patients get an idea of how long people with similar types of cancer live after diagnosis. The data is only an estimate, however, and does not include all variables, such as other medical conditions, lifestyle, etc. Overall survival is generally higher for NSCLC than for SCLC.
Using information from the SEER database, which is maintained by the National Cancer Institute (NCI), the ACS estimates 5-year relative survival rates. These rates are staged based on:
- Localized: The cancer has not spread outside the lung.
- Regional: The cancer has spread to nearby structures or lymph nodes.
- Distant: The cancer is detected in distant parts of the body, such as the other lung, liver, bones or brain.
Using data from 2010 to 2016, the ACS provides the following 5-year relative survival rate:
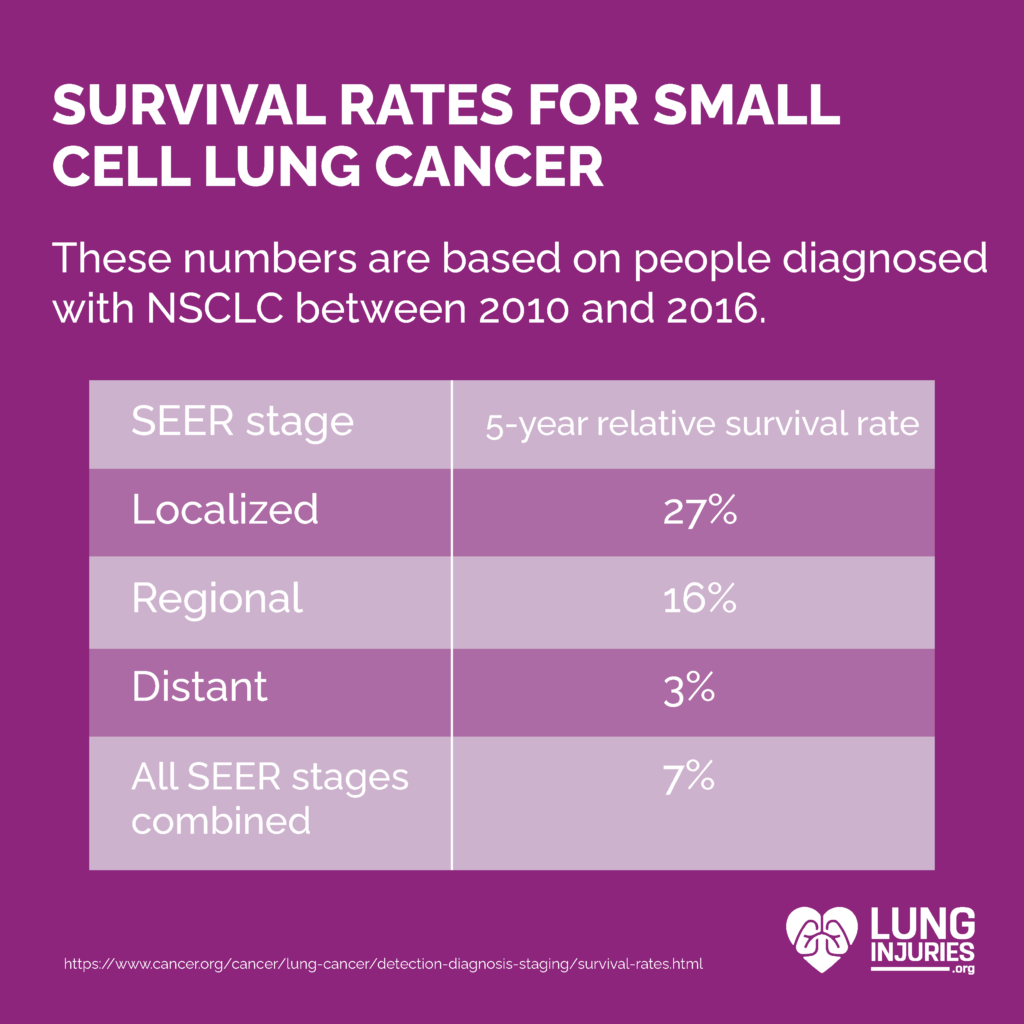
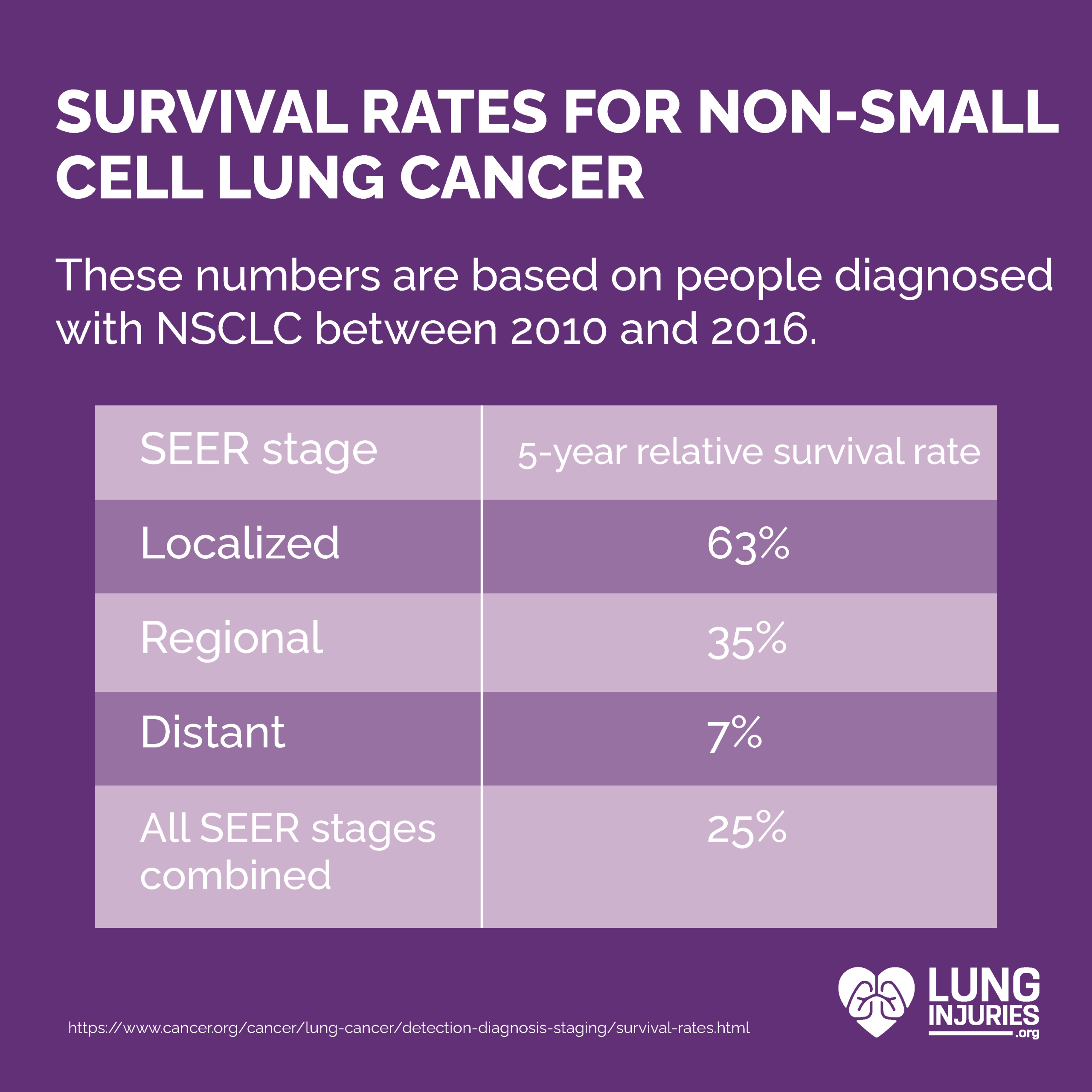
What these numbers mean is that someone with a 50% survival rate is 50% as likely as someone without cancer to live at least five years after diagnosis. Again, these are just estimates, and should not serve as a replacement for your doctor’s advice and prognosis.
Sources:
- https://www.cancer.ca/en/cancer-information/cancer-type/lung/statistics/?region=on
- https://www.cancer.ca/en/cancer-information/cancer-type/lung/risks/?region=on
- https://www.mayoclinic.org/diseases-conditions/lung-cancer/symptoms-causes/syc-20374620
- https://www.lung.org/lung-health-diseases/lung-disease-lookup/lung-cancer/learn-about-lung-cancer/lung-cancer-basics
- https://www.lungcancer.org/find_information/publications/163-lung_cancer_101/265-what_is_lung_cancer
- https://www.cdc.gov/cancer/lung/basic_info/what-is-lung-cancer.htm
- https://www.cancer.org/cancer/lung-cancer/about/what-is.html
- https://medlineplus.gov/smoking.html

